Cookie Policy: This site uses cookies to improve your experience. You can find out more about our use of cookies in our Privacy Policy. By continuing to browse this site you agree to our use of cookies.
AdipoGen Life Sciences
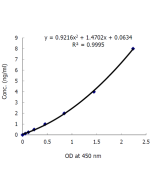
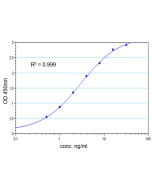
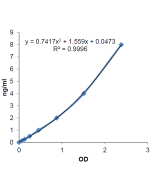
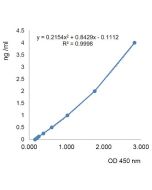
Insulin (human) ELISA Kit
| Product Details | |
|---|---|
| Synonyms | INS; Insulin A Chain & Insulin B Chain |
| Product Type | Kit |
| Properties | |
| Application Set | Quantitative ELISA |
| Specificity |
Detects human Insulin in serum, plasma and cell culture supernatant. |
| Crossreactivity | Human |
| Quantity |
1 x 96 wells |
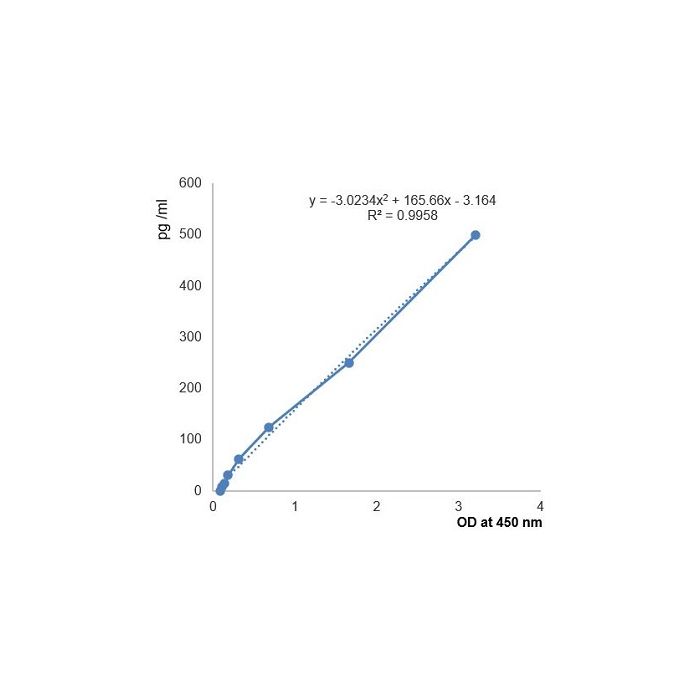
| Sensitivity | 10 pg/ml |
| Range | 7.81 to 500pg/ml |
| Sample Type |
Cell Culture Supernatant Plasma Serum |
| Assay Type | Sandwich |
| Detection Type | Colorimetric |
| Other Product Data |
UniProt link P01308: Insulin (human) |
| Accession Number | P01308 |
| Shipping and Handling | |
| Shipping | BLUE ICE |
| Short Term Storage | +4°C |
| Long Term Storage | +4°C |
| Handling Advice |
After standard reconstitution, prepare aliquots and store at -20°C. Avoid freeze/thaw cycles. Plate and reagents should reach room temperature before use. |
| Use/Stability | 12 months after the day of manufacturing. See expiry date on ELISA Kit box. |
| Documents | |
| Manual |
 Download PDF Download PDF |
| MSDS |
 Download PDF Download PDF |
| Product Specification Sheet | |
| Datasheet |
 Download PDF Download PDF |
Glucose is the main fuel for the human body and blood glucose values are tightly regulated in healthy individuals. Regulation of glucose uptake in cells is performed by the hormone called insulin which is glucose-responsively secreted from pancreatic β cells. When the glucose concentration in the blood is increased, insulin lowers it by increasing glucose uptake by muscle, liver and fat cells. Insulin is synthesized by β cells of the pancreas in the form of a single chain of three peptides B, C and A in the order: B-chain-C peptide-A-chain. The mature insulin consists of B-chain (30 amino acids) and A-chain (21 amino acids) linked by two inter-chain and one intra-chain disulfide bridge.
Insulin mediates its signal through insulin receptor (IR), but also through its highly homologous insulin-like growth factor 1 receptor (IGF1R). Binding of insulin on IR or IGF1R results in the phosphorylation of insulin receptor substrate 1/2 (IRS1/2) at its tyrosine residues and in the subsequent activation of two main pathways, the phosphoinositide3-kinase(PI3K)/AKT pathway and the mitogen-activated protein kinase (MAPK) pathway. The biosynthesis of insulin in the β cells of the pancreas is regulated by numerous mechanisms but is primarily stimulated by the presence of glucose and augmented by cAMP. Once secreted from the pancreatic β cells, insulin circulates in the bloodstream with an approximate half-life of 12 min. Numerous tissues and organs express the insulin receptor and various actions are initiated.
Insulin causes the translocation of GLUT-4 (the glucose transporter predominantly found in skeletal muscle and adipose tissue) from intracellular vesicles to the cell membrane and, thus, increases the rate of glucose entry for a given concentration into the target tissue. Insulin deficiency or the resistance of target tissues to insulin are referred to as variants of diabetes mellitus, which has become a serious contemporary health issue. Diabetes mellitus is subdivided into the categories insulin-dependent (type 1) and non-insulin-dependent (type 2), both of which can cause severe hyperglycemia. Immune cells express insulin receptors following activation and insulin mediates an anti-inflammatory effect in a range of clinical settings. So insulin also shapes the immune response during an infection.